I hope you enjoy my blog:
Choosing an Acupuncturist
Types of Acupuncture - (10 main Acupuncture schools)
The impact of diet choices on environmental health
Evidence that Wim Hof breath method works!
What is Yin Deficiency and What are Yin Supporting & Replenishing Foods
Choosing an Acupuncturist
Types of Acupuncture - (10 main Acupuncture schools)
The impact of diet choices on environmental health
Evidence that Wim Hof breath method works!
What is Yin Deficiency and What are Yin Supporting & Replenishing Foods
24th July 2021
Choosing an acupuncturist
Looking for a good acupuncturist?
Here are 7 questions you can ask and the answers you should be looking for
1. What are your qualifications and how long have you studied?
Although acupuncturists in the UK don’t need a university degree in acupuncture to practice, it is recommended that you choose can acupuncturist who has a degree or at least 4 years of education in the field. An education of less than 4 years in the field would not be sufficient to cover and integrate the knowledge of both the Eastern and Western medical traditions together with clinical practice make a good and effective acupuncturist.
2. Do you check pulse and diagnose internal organs?
Answer to look for: Yes!
the acupuncturist doesn’t diagnose from pulse, and possibly tongue, they aren’t an acupuncturist in the traditional sense. Instead, they do what is called “dry needling” which is a superficial practice. The approach does not apply the rich knowledge and experience of traditional acupuncture which seeks balance of the internal organs and they might end up draining your energy more than balancing your energy or giving you some.
3. Do you check the pulse after each needle insertion?
Answer to look for: Yes!
An acupuncturist with considerable experience knows that each needle insertion can affect the person differently in each moment in time. Consider, when you shoot the arrow on a target, you go and check to see if you succeeded or you need to calibrate better or aim differently. If the acupuncturist doesn’t do this, s/he cannot track the progress and effectiveness of the treatment and you may end up leaving the acupuncturist more drained of energy with the treatment being based more on theory (e.g. “this should work”) rather than reality (e.g. “that should have worked, I need to adjust”). Remember, after each needle insertion, your practitioner needs to re-check your pulse.
4. Can we have a brief telephone call so I can learn more about your practice?
Answer to look for: Yes!
An acupuncturist should be open to briefly speaking with you before treating you. Rapport is very important as an acupuncture session isn’t or really shouldn’t just be a matter of laying on a table while the acupuncturist inserts needles. It is a conscious energetic exchange.
It is common for traditional acupuncturists practicing Traditional Chinese Medicine (TCM) to put little emphasis or value on communication.However, I disagree with this approach. You, as a patient, should be able to have space to communicate your feelings, fears, concerns and expectations and have an acupuncturist that can listen, reflect and connect. It is important for the acupuncturist to be open and willing to communicate generously and help you understand your progress.
Make sure to speak to your acupuncturist on the phone beforehand to see if you have a rapport and sense as to whether s/he is the right healer for you.
5. Do you use Moxa/Moxibustion?
Answer to look for: Yes!
Moxa is one of the best tools that is used in acupuncture! In Japan practitioners get the same results with Moxa even without the actual acupuncture. If acupuncture moves the energy and works on the Yang level – then Moxa adds energy and works more on the Yin level and strongly tonifies in deficient and chronic cases. The best Moxa is direct or thread Moxa – a Moxa stick isn’t as accurate.
6. Can you cure me?
Answer to look for: I will do my best.
The acupuncturist is an instrument and you want one that will do his/her best to help your body to heal. However, your healing depends on other factors outside of the acupuncturists control. The acupuncturist must be aware that each person is individual and very often the prognosis depends on diet, lifestyle and mindset changes too.
7. How long will it take to get better? How many sessions do I need?
Answer to look for: it will take time a number of regular sessions to experience lasting improvement.Expect about 5-6 sessions to experience a real improvement.
Some people heal and progress quicker than others. Oftentimes, you might not always feel the difference during or right after the treatment, but you should feel more relaxed and some alleviation of certain troublesome symptoms. However, with acupuncture we are not targeting the symptoms – we are going deeper to target the root cause. This is why it can take time to heal.
If you want to see how Moxa works, take a look at my MOXA demo here and you may even want to try it for yourself at home!
5th September 2021
Types of Acupuncture
What Acupuncture schools are out there?
10 main acupuncture schools
When most people hear the word “acupuncture”, they assume it has something to do with inserting needles into the body. However, not all acupuncture requires the insertion of needles, such as Japanese Toyohari acupuncture or “Meridian Therapy” as the Japanese practitioners sometimes call it. In actuality, in traditional Chinese acupuncture, only 2 out of the 9 needles were supposed to be inserted.
Bear in mind that given the long history of acupuncture spanning thousands of years, needles weren’t always manufactured so thin and fine to be able to be inserted into the skin without causing a serious wound.
Acupuncture is underpinned by pulse taking and a holistic understanding of the organs of the body – it is one of the longest traditions of medicine and integrates key concepts such as “5 Elements” and “Yin/Yang”. If it were not for immense and complex knowledge and methodology which determines why a needle is inserted or not in particular place, acupuncture would be just like shooting arrows onto a target (the body).
Historically speaking, almost everyone associates acupuncture with its Chinese origins, but a lot of religious and philosophical knowledge was transferred to China from India. For example, could there in fact be a Sanskrit connection between the roots of acupuncture and the Nadis – the identification of energy lines similar to meridians mentioned in Ayurvedic and other Vedic traditions? It would also be interesting to know what acupuncture was like before the communist cultural revolution of Mao Zedong unified many different Chinese branches and schools into Traditional Chinese Medicine (TCM).
Before we look at the main schools of acupuncture, it’s important to consider the main features that connects them all:
- Pulse diagnosis
- Identifying “meridians” - acupuncture points (of which there are around 360+)
- Theoretical knowledge, understanding and application of concepts such as Yin-Yang, 5 Elements, and Organ Theory.
- Understanding that if there is an excess of energy – Qi, there must be a deficiency (lack) somewhere too – and the relationship that these two have is crucial in the clinical application of acupuncture.
In acupuncture, the practitioner has to be able to differentiate the diagnosis not from the theory or symptomatic presentation, but from pulse (and tongue) checking.
Acupuncturists are able to diagnose the state of all internal organs and assess if they under/over function. To put it simply, acupuncturists give or take energy - Qi - to/from organs by stimulating relevant meridians of the organ. One has to understand the deep interconnectedness and holistic relationship of the body and organs before one can attempt to diagnose and treat with acupuncture.
If you go to your GP, osteopath or other practitioner for acupuncture and they don’t carry out a pulse diagnosis of internal organs, then most likely you haven’t had acupuncture. Instead, you have had dry-needling, which is just a few needles stuck into you. This is actually only muscle stimulation, and should not be associated with the assessment of the internal organs by the pulse and tongue check underpinned by the deep knowledge and tradition of acupuncture. Without checking the pulse consistently during the treatment, the practitioner is at best relying only on theoretical and empirical knowledge of how needling particular acupuncture point might be helpful for the local muscle – but not to the whole body.
As we are all different sizes and shapes, each needle insertion should be double checked and followed with pulse taking to see if the intention and energy shift was accurately achieved. If pulse checking isn’t done after each needling – what could happen is that the person might end up not benefiting from acupuncture – as the acupuncturist is only practicing the theoretical medicine.
Therefore, always make sure you go to an acupuncturist that checks your pulse after each needle insertion or manipulation.
Now let’s have a look at the most common acupuncture schools and traditions and the differences between them. Try noticing that some schools are more pulse-orientated (going deeper into the origin of the issue in the body) and others more symptomatic.
1. Traditional Chinese Medicine (TCM)
TCM is the most generally known and applied type of acupuncture out there. It was coined after Mao Zedong’s cultural revolution where he ordered that the variety of ancient and specific Asian traditions of acupuncture be compiled and to a degree, “unified” in one place.
With this unification of the various acupuncture traditions, many smaller schools and traditions were erased and some rich cultural and spiritual traditions weren’t included, due to communism’s distrust of spirituality and anything that was old and traditional. The place of spirituality in acupuncture can be seen in many terms still used in TCM such as spirit, spiritual, ghost – but in the TCM, they don’t quite have the same application as they used to and are used more empirically.
Even though the knowledge and tradition of acupuncture in Asia is so ancient and vast, many of them used the most common laws, rules and concepts which are now used by TCM such as:
- 28 Pulse qualities Based on Depth, Width, Strength, Shape, Rhythm, Rate
- 6 Stages
- 4 Levels
- 8 Extraordinary Channels
- 8 Principles
- Yin & Yang
- Six Extraordinary Fu
- Mother/Child
- 5 Elements and its application and Acupuncture points division
- 12 Officials/Organs
- Organ clock
- Vital substances: Jing – Essence, Qi - Energy, Xue - Blood, Shen – Spirit, Jin Ye – Fluids
2. Five (5) Element Worsley Acupuncture
This style of acupuncture was found by JR Worsley who combined different acupuncture styles and created his own style which divides people by a particular predominating element or what he called CF – Causative factors, which is one of: Fire, Water, Earth, Metal or Wood.
The system is based on observing the colour, sound, emotion and odour (“CSEO”) of a person which then determines which one of these elements apply. Treatment is done mainly on the meridian related to the relevant element. Other meridians aren’t treated apart from Bladder Back transporting Shu points and Chest-Kidney points.
Worsley also included into his system a number of unusual and not very well known tools to create a much more dynamic acupuncture style. So although the CSEO diagnosis relies on observation of the whole body, the following dynamic tools may also determine diagnosis and very much includes the pulse diagnosis. These are:
- Law of Husband & Wife or Left/Right pulses block
- Possession or Internal & External dragons ( ID’s & ED’s )
- CV/GV or Ren/Du block
- Meridian blocks (entry/exit blocks)
- Aggressive energy drain
- Energy transfers
Worsley’s greatness was in bringing these unusual systems of treatment and combining them into what is in the West called “5 element acupuncture”.
However, what is generally called the “law of 5 element” is just one of the acupuncture tools used across ancient medicine – even as a base of Ayurvedic 3 Doshas and in shamanic and witchcraft medicine as pentagram for tools of transformation and development of base elements.
3. Hicks – Integrated Acupuncture (TCM and 5 Element Acupuncture)
John Hicks was a student of JR Worsley and he combined TCM and Worsley’s style of acupuncture. The traditional knowledge that Worsley was selective about, Hicks used and added to, creating whole sets of principles on how to combine the two schools.
He is/was a master teacher and the integrated Hicks acupuncture is by far the best combination of the two rich traditions of Worsley and TCM, combining the best parts of them. It adds more clarity and wider application to Worsley’s tools. As we already covered TCM and Worsley’s 5 Elements above, we will not go into detail on Hicks’ approach which is a genius combination of the two.
4. Toyohari Acupuncture (based on Meridian Therapy)
Toyohari was established on the basis of Meridian Therapy. Most of the practitioners in its country of origin – Japan – were blind, and so developed a greater sensitivity to palpation which determined the diagnosis and treatment. Toyohari does not generally involve the insertion of needles – 95% of the time it does not! Yes you read this correct – needles doesn’t need to be inserted in acupuncture – but then you rightly ask – shouldn’t this practice be called something else? The founders of this system went into decades of study and compared the old traditional Chinese scripts and sifted through what works and what doesn’t in practice. They realised that in order to get the patient better, one doesn’t need to insert the needle. And where as in Hicks, Worsley and TCM style – one has to wait for the sensation of De Qi – or what sometimes patient feels as electric shock after needle insertion, in Toyohari, the practitioner can feel the sensation of Qi change in his own body. Because of this, the Toyohari practitioner has to be much more developed and attuned in pulse taking, meditation and energy awareness/manipulation.
Apart from also integrating the wisdom of TCM, this system has what are called primary and secondary systems of treatment. The primary system is the Root treatment – which is uniquely tested by comparing which organ/element and its mother or preceding element is lowest on the pulse. This is done on a generating cycle. Then this element is tonified or given energy. Then the controlling cycle is used and depending if its full or empty – is either drained or tonified.
Secondary treatments involve additional energy giving and rebalancing tools like:
- Naso, Muno
- Shigo
- Kikei
- Okyu moxa
- Micro Blood letting
- Release of Jitsu and Jya ki/Sha Qi
It is interesting to point out that the location of acupuncture points is not always exactly at the agreed anatomical locations, but they are the starting point for what is called the ‘alive point’. The revealed alive point is differentiated by thermal & tactile distortions which are felt out by the practitioner and this is where Japanese acupuncture and particularly Toyohari practitioners are surprised to see TCM & Chinese practitioners not touching and feeling the area of insertion first which is necessary to identify the alive point, but instead using the points on the body like a dart board.
On top of all these very refined tools and approaches, the three things stand out very uniquely in this profound school. First is its super-refined and extremely sensitive skill of holding the needle or ‘Oshide’ (with the non-insertive hand). This needling becomes more or less a meditation and the practitioner has to develop a deep sense of awareness of energy in their own body. The needling application with what is called as clearing Sha-qi or dirty Qi is extremely unique. Also, no other style of acupuncture combines Tonifying and reducing in one needling action. Second is the training of the acupuncturists in this style – which was established by Mr Kozato – and it is pulse checking is able to speed up the development of the practitioner by many years as each part of the needling is checked by several teachers who all form a chain reaction style of pulse taking, thus giving a valuable feedback to the practitioner. This means that advanced practitioners can tell from pulse taking if the practitioner who is needling is tense in their body or their needle is at a wrong angle or too deep or just not quite right. Wouldn’t you want to be treated by a practitioner who had had a teacher/acupuncturist who is able to determine by touching the pulse of a patient – if the student/practitioner is tense or thinking what to buy for dinner? This is how Toyohari practitioners are trained in Kozato training.
Acupuncture in Japan used to be and still is often the art of blind practitioners and they raised the standard very high for rest of the other acupuncture schools with their ability to send and receive the signals from and to a body.
The third is the needle thinness comparison. Generally, Toyohari practitioners are using 0.14-0.20 mm needles, most of the time silver and at times gold, as these purer metals are conducting the energy/qi differently to stainless steel. Most of the other schools start with 0.25 mm thickness and could go all the way up to 40 mm. The understanding is that the thicker the needle – more of energy/qi could be leaked or wasted.
5. Japanese Acupuncture
Japanese acupuncture is primarily known by its subtle and soft needling. It uses the same wisdom as TCM but adds slightly different treatment applications that are based more on tonifying the organ with the least amount of the energy and thus going to the root of the problem (root treatment). This system tries to establish balance in the pulse. Where there is excess, it reduces it, and where there is deficiency – it tonifies or supplements it.
Generally, there are many schools of acupuncture in Japan and they weren’t all unified into what would be Traditional Japanese Acupuncture. The most well-known are Manaka, Sawada, Akabane, Matsumoto, Fukushima but there are many more, each providing unique system of the application.
It is a given that preliminary palpation and a soft touch is what differentiates this style from TCM. Nevertheless, it is still very much a tradition of acupuncture which is firmly based not only on palpation and meridians, but also on pulse taking and the rich Chinese wisdom traditions.
Honorary mention should be given to one of the tools of Japanese practitioners – Shiatsu – which is advanced meridian massage which doesn’t involve pulse diagnosis or needles. This amazing skill is just a side skill that was later developed into its own school.
It was also Japanese practitioner Waichi Sugiyama who first introduced the needle tube-guide – allowing the use of these thinner and finer needles.
6. Dr Tang and Dr Tung
This system is based on symptomatic presentation and the treatment of pain and Musculo-skeletal issues. However, this could be a gross understatement as it does use the rich knowledge of Chinese medicine, the organs and its relationship with 5 Elements. This was one of the system’s that was saved from the Communist cultural revolution and was preserved in family dynasties, its secrets only given to a few special ones or blood family but which has nowadays becomes more widely spread.
Generally, if this system is used by a practitioner who doesn’t use pulse checking and balancing and just concentrates on the pain, it is just a sub-system of acupuncture and could be classed as very advanced dry needling. However, if it is used by experienced acupuncturist who uses one of the aforementioned schools, it could be seen as a useful tool to deal with secondary treatment – removing symptoms, which comes after what is called a Root treatment, or a treatment trying to get to the original imbalance.
7. Korean and micro-systems acupuncture
Generally, these are easier and simpler acupuncture styles where the practitioner doesn’t normally diagnose by the pulse but just by the symptoms and observation. It is normally limited to hands and feet and the whole body is used with the theory of micro/macro system or cosmos – meaning that the whole body could be found within the hand or foot. It is generally practiced as a side treatment. It could be classified as dry-needling if it doesn’t use the pulse taking and the understanding of the knowledge of meridians.
8. Auricular acupuncture
This isn’t really acupuncture, but more of a very simple application of dry needling on the ear. The ear has a map linked to / identified with approximate areas of the body. These points are either stimulated by needles or by seeds on a plaster and further massage.
The mapping of the ear was largely developed by Dr. Paul Nogier.
Auricular acupuncture is famous for its NADA protocol – used for detoxification and quitting and addictions of alcohol, drugs and smoking – where commonly several Yin organs plus sympathetic nervous system is punctured/stimulated.
There isn’t any pulse checking in general auricular application of acupuncture and it is more or less safe and could be used at home by anyone with simple mustard seeds, a plaster and a map of the ear.
9. Stems and branches of acupuncture
According to the “Stems and Branches” theory, man reflects the universe / cosmos – a small part (man) which mirrors the whole (universe). This means that the same rules that influence nature on the macro level, influence man in a similar way on the micro level.
This system of acupuncture is one of the many that has barely survived the onslaught of communist China’s massive movement towards a more unified system of practice. This system is unique as it is premised on the idea that energy – Qi – moves differently across the meridians depending on the time of the year. It relies on a rich history of traditional Chinese knowledge and combines it with planetary and astrological wisdom. The result is a constitutional treatment tailored directly for your birth place, time and date.
If the practitioner uses pulse taking and not just theoretical knowledge of 10 heavenly stems (planets) and 12 earthly branches (seasons, months, hours, minutes), the results of a treatment can be very promising. If, however it is only theoretical calculation without checking pulse and (tongue) the result might not be as helpful.
10. Dry needling
Under this style belongs all following: dental, medical, electro, head, scalp, neurological and animal acupuncture.
When a child comes to garden and tries to penetrate the earth with little toys, and the parent jokes, “you are a gardener, aren’t you?”
This is the analogy that could be given to anyone who takes a needle and sticks it into the body without understanding first the rich theory of Chinese wisdom, pulse diagnosis and meridians. For acupuncture to be acupuncture – one must understand the theory of organs and the different pulse qualities (not just the pulse rate). These are the following pulse qualities: Depth, Width, Strength, Shape, Rhythm and Rate. These determine 28 pulse types. In order to understand what each one means, one needs to take a deep dive into theory, application and practical clinical knowledge of many years.
No doubt that when osteopath or GP sticks needle into the spine – and calls it acu-puncture – he might relax some nerves and muscles, and probably influence a soft tissue or ease some pain. However, this in no way is compared with vast benefits of a practitioner who is able to understand pulse checking and its organ application/ diagnosis.
Scalp/Head/Neurological acupuncture
This acupuncture uses a needle to stimulate skin on the top of the skull – which is shown to have brilliant application with symptomatic presentation of many neurological conditions.
Yamamoto New Scalp Acupuncture
This tradition deserves special mention as it uses very rich mapping system around the neck and head and has excellent application for neurological and Muscular-skeletal issues.
Electro acupuncture
This is a tool that could numb pain and works mostly as a tool of an acupuncturist or a body-worker who does want to release some of the symptoms. However, a person with deep knowledge of meridians would be able to do the same just with non-insertive Japanese needle. Electro-acupuncture could also confuse the delicate balance of Qi whereas a specific Qi manipulation of a needle, specially by practitioner who is fully present and has her/his own meditative and qigong/neigong practice, sends very clear and natural command that the body can understand.
Veterinary animal & pet acupuncture
This type of acupuncture has been widely used on horses in Chinese ancient military and later the principles of meridians was drawn on the body of any animal/pet.
It is dry needling and theoretical application that is very useful but it is extremely difficult to be able to do any pulse checking on animals. But there is no harm in using it, actually opposite – vets and animal doctors have been using it for pain release and confronting some common ailments.
Conclusion
To sum it up, if a practitioner doesn’t check your pulse and analyses your internal organs, they don’t do real acupuncture – but what is at best called Dry Needling and at worst, some type of dart game. Most dart games are meant to score the win – which in this case is pain numbing, but doesn’t go to the root/origin cause of the illness.
13th of September 2021
The impact of diet choices on environmental health
A number of studies have now highlighted the impact of our diet choices on environmental health. The Intergovernmental Panel on Climate Change (IPCC) report warns about the dire consequences of the projected global warming of 1.5 °C above pre-industrial levels, which could happen in only 12 years time. This includes extreme heat, increased and more frequent flooding and droughts, rising sea levels, species loss and extinction and risks to human health, livelihoods, food security, water supply, human security, and economic growth.
The current global food and agriculture system is a major driver of climate change, water pollution, land degradation, loss of wildlife and biodiversity, deforestation and ocean destruction. Animal agriculture produces more greenhouse gas emissions than all forms of transportation combined. One of the most comprehensive analyses of the global farming system, assessing all aspects of the food chain from ‘farm to fork’, concluded that shifting to a plant-based diet would have the most impact on planetary health than any other driver of climate change (1). Meat and dairy production uses 83% of farmland and produces 60% of agricultural greenhouse gas emissions, whilst only providing 18% of calories and 37% of protein. Even the production of meat and dairy with the lowest environmental footprint is less sustainable that the worst performing plant food source. Fresh water fishing and grass fed beef, generally considered more sustainable, was found to have a greater environmental effect than once thought and creates more greenhouse gas emissions than any plant food source. Further studies have examined the impact of shifting towards plant-based diets on both human and environment health and concluded definitively that it would provide combined benefits (2). Plant-based diets could reduce green house gas emissions by 56% and other environmental impacts of the food system by 6-22%, whilst at the same time improving the nutritional quality of our diet and significantly reducing the burden of chronic disease and reducing premature mortality by 22%.
Most recently, the Eat-Lancet Commission has developed global scientific targets that brings together recommendations for a global healthy reference diet, produced from sustainable food systems, to ensure that the United Nations Sustainable Development Goals (United Nations, 2016) and Paris Agreement (United Nations Convention on Climate Change, 2015) are achieved (3). As mentioned previously, the reference diet consists mainly of whole plant foods, with low amounts of animal-derived and processed foods. It estimates that the global adoption of this reference diet would prevent around 11 million deaths a year or 23% of adult deaths.
Another major issue with our current food system and threat to global health is the widespread use of antibiotics in animal agriculture. Around 40-70% of all antibiotics globally are sold for use in animals and it has been recognised for many years that agricultural use of antibiotics is a major contributor to antibiotic-resistant infections in humans. We are entering a post-antibiotic era where it is no longer unusual to be treating patients with infections for which there are no suitable antibiotics. A review of antibiotic resistance commissioned by the UK Prime Minister, reported in 2016 (4). It suggested that globally, 700,000 lives are lost annually from antibiotic-resistant infections and by 2050 the number could be as high as 10 million. One of its 10 recommendations is the reduction of antibiotic use in animal agriculture. However, with the increasing industrialisation of food production and the growing demand for meat, this will be impossible to achieve without Governments working together. This is a global issue, which requires a global solution, and reducing antibiotic resistant organisms in our food system needs to be a priority.
Despite the widespread use of antibiotics in animal agriculture, food-borne infections (bacteria, viruses, protozoal) continue to be a major cause of morbidity and mortality worldwide, with most due to contamination of animal-derived foods or plant-foods that have been contaminated by the manure of food animals. One of the most comprehensive studies of the worldwide burden of food-borne illnesses estimated that in 2010 there were 582 million cases of infection caused by contaminated food, with 351,000 deaths (5). In 2018, there were nearly 50,000 cases of foodborne infection in the European Union with 1 in 3 cases caused by Salmonella, mainly linked to the consumption of eggs
Most recently, the Eat-Lancet Commission has developed global scientific targets that brings together recommendations for a global healthy reference diet, produced from sustainable food systems, to ensure that the United Nations Sustainable Development Goals (United Nations, 2016) and Paris Agreement (United Nations Convention on Climate Change, 2015) are achieved (3). As mentioned previously, the reference diet consists mainly of whole plant foods, with low amounts of animal-derived and processed foods. It estimates that the global adoption of this reference diet would prevent around 11 million deaths a year or 23% of adult deaths.
Another major issue with our current food system and threat to global health is the widespread use of antibiotics in animal agriculture. Around 40-70% of all antibiotics globally are sold for use in animals and it has been recognised for many years that agricultural use of antibiotics is a major contributor to antibiotic-resistant infections in humans. We are entering a post-antibiotic era where it is no longer unusual to be treating patients with infections for which there are no suitable antibiotics. A review of antibiotic resistance commissioned by the UK Prime Minister, reported in 2016 (4). It suggested that globally, 700,000 lives are lost annually from antibiotic-resistant infections and by 2050 the number could be as high as 10 million. One of its 10 recommendations is the reduction of antibiotic use in animal agriculture. However, with the increasing industrialisation of food production and the growing demand for meat, this will be impossible to achieve without Governments working together. This is a global issue, which requires a global solution, and reducing antibiotic resistant organisms in our food system needs to be a priority.
Despite the widespread use of antibiotics in animal agriculture, food-borne infections (bacteria, viruses, protozoal) continue to be a major cause of morbidity and mortality worldwide, with most due to contamination of animal-derived foods or plant-foods that have been contaminated by the manure of food animals. One of the most comprehensive studies of the worldwide burden of food-borne illnesses estimated that in 2010 there were 582 million cases of infection caused by contaminated food, with 351,000 deaths (5). In 2018, there were nearly 50,000 cases of foodborne infection in the European Union with 1 in 3 cases caused by Salmonella, mainly linked to the consumption of eggs
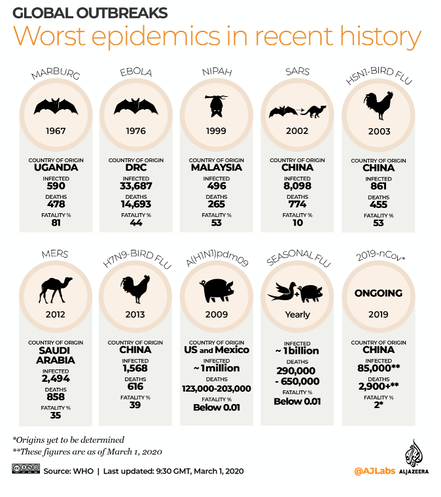
Industrialisation of animal farming along with the wildlife trade and habitat destruction has led to the perfect conditions necessary for the transmission of novel infections, mostly viruses, from animals to humans (zoonoses). Virtually all epidemic and pandemic infections, going back to the 1918 influenza pandemic, can be traced back to transmission from animals and resulting from our farming practices and the use of animals as food. In 2020, the entire world has been overwhelmed by a pandemic caused by the virus SARS-CoV-2, leading to COVID-19, with catastrophic consequences. The initial transmission of the virus to humans is thought to have occurred in the live animal markets of Wuhan, China with the Pangolin, one of the most widely traded wild animal, being the intermediary host. You can read this excellent review on Food and Pandemics produced by ProVeg.
Figure 1: Origins of infectious epidemics in the 20th and 21st century.
We are now accelerating towards the sixth mass extinction event with record number of animal species being lost (6). The Living Planet Report from the WWF shows that the planet’s wildlife populations have now plummeted by 68% since 1970, and there are no signs that this downward trend is slowing. The report states 'With global action to protect wildlife, produce food in better ways, and change what we choose to eat, we can turn things around'. This global action requires a shift to a plant-based food system. This is now undisputed.
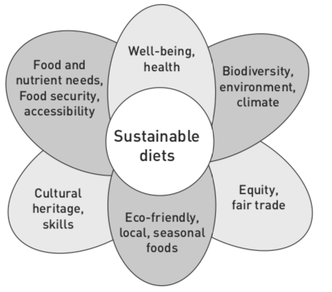
Of course a sustainable diet is much more than one that is optimal for health and the environment. Other socioeconomic factors are just as important. The Food and Agricultural Organization (FAO) has a definition that includes aspects of food and nutrition security, culturally acceptability, accessibility, economic fairness and affordability (Figure 2). Pamela Mason and Tim Lang, in their book ‘Sustainable diets’ consider the following six core values: quality (including taste, seasonality, cosmetic); social values (pleasure, religion, animal and human justice); environment; health; economy (food security, affordability, jobs and working conditions); and governance (science and technology, democratic accountability, fairness) (7). They also highlight the issue of food waste, which in itself is unsustainable. For example, the EU food waste is 89 million tonnes a year, worth about £950 per household (8). Globally, approximately a third of food is wasted across the supply chain with 70% of this waste occurring in the home (9). The authors accept that there will be country-based differences in what a sustainable diet may be due to socioeconomic factors and individual foods choices need to be considered in the context of the wider food supply chain. However, they conclude a sustainable diet will be mainly centred on minimally processed plant foods with only small amounts of meat, fish and dairy.
Figure 2. Key components of a sustainable diet FAO 2010
It is encouraging to see that Government and national and international organisations are increasingly considering aspects of sustainability when making dietary recommendations. Some countries such as Germany, the Netherlands, Qatar and Brazil have produced sustainable dietary guidelines. The Public Health England 2016 dietary guidelines, called the Eatwell guide, considered the environmental sustainability of its recommendations and was able to show that adherence to the Eatwell dietary guide would have a lower environmental impact than the typical UK diet (10). The BDA (the association of UK dietitians) has launched its One Blue Dot campaign, a project aimed at promoting environmentally sustainable diets and providing toolkits for its members to use when advising patients and clients. Most recently, the Health Canada dietary guidelines not only emphasise and recommend an environmentally sustainable diet centred around whole plant-foods but also emphasises the importance of practical food skills and the importance of creating supportive environments for healthy eating, such that nutritious food is affordable and accessible to all (11).
Recommendations for fish consumption are where health and environmental considerations diverge. Most dietary guidelines recommend the consumption of fish once or twice a week, including the recently published Eat-Lancet commission reference diet. The regular consumption of fish does have positive health impacts, predominantly because it is replacing other less healthy foods, such as red and processed meat in the diet, and is a source of unsaturated fats, including long chain omega-3 fatty acids (12). Whether the addition of fish to a predominantly plant-based diet improves health outcomes above and beyond the benefits of eating whole plant foods is not known. However, it is not thought to be necessary and nutritional requirements can be met without consuming fish. Essential long chain omega-3 fatty acids are the mostly commonly cited reason to continue to consume fish. However, they can be obtained straight from the source, marine algae, or from the precursor short chain omega-3 fatty acid found in plant-foods, including walnuts, chia and flax seeds (13). For a global population of over 7 billion to eat fish 1-2 times per weeks is unlikely to be sustainable given that 90% of world fish stocks are fully or over-exploited from fishing (14). In addition, there are concerns over mercury (15) and other fat-soluble pollutant (polychlorinated biphenyls and dioxins) contamination of fish and shellfish, particularly larger fish that are higher up the food chain (16). Mercury in particular is associated with neurological toxicity.
The way our food is produced is also of concern for environmental health. Our current food system is dominantly based on tillage agriculture, which has become progressively intensified and industrialised. The majority of our food production is thus based on intensive mechanical soil disturbance and excessive use of agrochemicals. This has resulted in large-scale soil erosion and land degradation. Some 10 million hectares of cropland is being lost annually due to intensive tillage agriculture used to produce plant-based products for both human and animal consumption. Thus, there is a need not only to drastically change our diet, but also to move away from the degrading tillage agriculture into Conservation Agriculture, which is an ecologically sustainable way of growing and producing plant-based foods. This will be further explored in the lecture.
The international community has called Health Professionals to action. The Eat-Lancet commission urges health professional to consider both health and environmental sustainability when counselling patients about diet and recommends advising the shift to more plant-based diets. The World Organization of Family Doctors (WONCA) have published a “Declaration Calling for Family Doctors of the World to Act on Planetary Health". This involves advising patients to transition to a more plant-based diet in line with the Eat-Lancet planetary health diet.
It is not only important to shift to a plant-based diet but also to increase the variety of foods in the diet. The WWF, a leading independent conservation organisation, have produced a report highlighting the need to diversify our diet. They report that 'Globally we rely on a small range of foods. This negatively impacts our health and the health of the planet. Seventy-five percent of the global food supply comes from only 12 plant and five animal species. Just three (rice, maize, wheat) make up nearly 60 percent of calories from plants in the entire human diet. This excludes many valuable sources of nutrition. While people may be getting sufficient calories, these narrow diets don’t provide enough vitamins and minerals. Dietary monotony is linked to a decline in the diversity of plants and animals used in and around agriculture (agrobiodiversity), threatening the resilience of our food system and limiting the breadth of food we can eat. Since 1900, a staggering 75 percent of the genetic plant diversity in agriculture has been lost. In most Asian countries, the number of rice types grown has decreased rapidly from thousands to a dozen. In Thailand, for example, the 16,000 varieties once cultivated have dropped to just 37 varieties. In the past century, the United States has lost 80 percent of its cabbage, pea and tomato varieties. This dependence on a limited pool of crop species leaves harvests vulnerable to pests, diseases and the impact of climate change. Farming a narrow range of crops using intensive methods can have serious repercussions on our fragile natural ecosystems. Monoculture farming, which is the repeated harvesting of a single crop, and over-reliance on animal-based foods are threatening food security. Monoculture farming can deplete nutrients and leave soil vulnerable to the build-up of pests and pathogens. This requires applications of fertilisers and pesticides that can, if used inappropriately, damage wildlife and leach into water systems. Many types of birds, animals and wild plants cannot thrive in biologically degraded landscapes.'
Download the full report, which highlights 50 foods we should eat more of because they are nutritious and have a lower impact on the environment, whilst increasing the diversity of our diet and farming systems. Not all of these foods are currently easily accessible but by making a conscious choice to consume more of these foods we may be able to help safeguard these foods for future generations.
REFERENCES
1. Poore, J. and Nemecek, T. (2018) ‘Reducing food’s environmental impacts through producers and consumers’, Science. doi: 10.1126/science.aaq0216.
2. Springmann, M. et al. (2018) ‘Health and nutritional aspects of sustainable diet strategies and their association with environmental impacts: a global modelling analysis with country-level detail’, The Lancet Planetary Health. doi: 10.1016/S2542-5196(18)30206-7.
3. Willett, W. et al. (2019) ‘Food in the Anthropocene: the EAT–Lancet Commission on healthy diets from sustainable food systems’, Lancet, 6736, pp. 3–49. doi: 10.1016/S0140-6736(18)31788-4.
4. United Kingdom Department of Health (2013) UK Five Year Antimicrobial Resistance Strategy 2013 to 2018, Department of Health. doi: 10.1186/s41021-015-0014-8.
5. Kirk, M. D. et al. (2015) ‘World Health Organization Estimates of the Global and Regional Disease Burden of 22 Foodborne Bacterial, Protozoal, and Viral Diseases, 2010: A Data Synthesis’, PLoS Medicine. doi: 10.1371/journal.pmed.1001921.
6. Gerardo Ceballos, Paul R. Ehrlich, Peter H. Raven (2020) 'Vertebrates on the brink as indicators of biological annihilation and the sixth mass extinction', Proceedings of the National Academy of Sciences, 117 (24) 13596-13602; DOI:10.1073/pnas.1922686117
7. Mason, P. and Lang, T. (2017) Sustainable diets: How ecological nutrition can transform consumption and the food system, Sustainable Diets: How Ecological Nutrition Can Transform Consumption and the Food System. doi: 10.4324/9781315802930.
8. EU Committee (2014) ‘Counting the Cost of Food Waste: EU Food Waste Prevention’, Authority of the House of Lords. doi: 10.1111/j.1365-313X.2010.04415.x.
9. Gustavsson, J. et al. (2011) Global food losses and food waste: extent, causes and prevention, Interpack2011: Save Food! doi: 10.1098/rstb.2010.0126.
10. Reynolds, C. J. et al. (2015) ‘Greenhouse gas emissions associated with sustainable diets in relation to climate change and health’, Proceedings of the Nutrition Society. doi: 10.1017/S0029665115003985.
11. Health Canada (2019) ‘Canada’s Dietary Guidelines’. Available at: https://food-guide.canada.ca/static/assets/pdf/CDG-EN-2018.pdf (Links to an external site.).
12. Food and Agriculture Organization of the United Nations/World Health Organization (2010) Report of the joint FAO/WHO expert consultation on the risks and benefits of fish consumption, FAO Fisheries and Acquaculture report n.o 978
13. Simopoulos, A. P. (2002) ‘Omega-3 fatty acids in wild plants, nuts and seeds’, in Asia Pacific Journal of Clinical Nutrition. doi: 10.1046/j.1440-6047.11.s.6.5.x.
14. FAO (2016) The state of world fisheries and aquaculture, The State of World Fisheries and Aquaculture 2016. doi: 92-5-105177-1.
15. WHO, W. H. O. (2017) ‘WHO | Mercury and health’, Fact Sheet n 361.
16. Hall, R. H. (1992) ‘A New Threat to Public Health: Organochlorines and Food’, Nutrition and Health. doi: 10.1177/026010609200800103.
15th of September 2021
Evidence that Wim Hof breath method works!
Did you know that practices as simple as breathing & taking cold showers can save and improve the quality of your life?
Wim Hof proved it many times!
In 2011, Wim Hof checked into a research lab at the Radboud University Medical Center in the Netherlands where researchers injected him with an endotoxin derived from E. coli. Now E. coli is a bacteria that usually lives in the intestines of people but strains can cause severe illness including stomach cramps, bloody diarrhoea, vomiting, nausea, headaches and fever.
Following the injection of E. coli into his veins, Wim Hof practiced his now infamous breathing technique. The power of his breathing allowed him to voluntarily influence and strengthen his autonomic nervous system and immune response and despite exposure to the noxious endotoxin, he was fine. Wim Hof was able to demonstrate the power of the mind and breathe in countering certain illness – something that was until then a myth.
Of course, Wim Hof has been training his breathe, body and mind for years – most of his life in fact. One can easily assume he’s an anomaly and not reflective of the general population. Wim Hof disagreed with this assumption, insisting anyone could do what he did. So, in Wim Hof style he set out to prove it.
The Radbound University researchers and Wim Hof came up with a new experiment. In 2014, they invited 24 healthy male volunteers to participate in the new experiment. The group of men were randomly split into two groups – a Wim Hof Group and a control group. The Wim Hof group set off on a retreat with Wim Hoff where for 10 days they learned Wim Hof’s techniques – mainly breathing practices and cold exposure. The control group received no training. After the 10 days, all the men returned to the lab and like Wim Hof before, they were injected with an E. coli endotoxin.
Can you guess what were the results?
The Wim Hof Group experienced no illness. The breathwork and cold exposure helped them keep their heart rate, temperature, and immune response within the normal range, like they haven’t been exposed to serious poison. Their anti-inflammatory mediators were 200% higher, while pro-inflammatory mediators were 50% lower than the control group. The control group unfortunately suffered the awful symptoms that arise from E. coli exposure.
Wim Hof and the researches at Radbound University proved that breathwork and cold exposure can keep us healthy and more than that, make us healthier and stronger than we otherwise would be.
Wim Hof has gone on to show further just how powerful our bodies can be, if we do the work. Or as he would say, if we get high on our own supply. Through consistent practice, Wim Hof has shown he can activate and control by his parts of his brain associated with pain suppression and wellbeing. In the 2018 experiment, he was able to release in his own brain opiates/cannabinoids which decreased sensitivity to the external environment and promoted euphoria and wellbeing.
In 2019, a randomised controlled trial of 24 patients suffering from Axial Spondyloarthritis was conducted. It was meant to prove what everyone already knew – that Wim Hof’s method is safe. The results also showed that there was significant drop in inflammation (ESR levels & ASDAS-CRP) in the group practicing Wim’s style of breathing and cold exposure.
Conclusion:
You may now be asking yourself, “why isn’t my GP telling me to breathe and have cold showers?”
I can’t answer that. The medical establishment cannot usually keep up with these advances and perhaps, they appear too easy. Yet, most people would still choose a pill over making the lifestyle change required to adopt and integrate these practices.
I can help you though. I often coach my clients to adopt practices that support their health goals. Breathing is a proven way to empower your body and immune system, but also help you support your mental and emotional wellbeing. I can coach you through the breathing and work out how you can adopt it within your lifestyle.
It is time to take these ancient yogi practices and make them a part of modern health!
28th of September 2021
What is Yin Deficiency and What are Yin Supporting & Replenishing Foods
According to Chinese medicine, the body is part of greater balance of Yin & Yang. This concept is a theory of equilibrium. The Yin & Yang are like two opposites working together and complementing each other, present in everything we see or understand. It is hard to translate Yin into Western terms, but the concept might be easier understood by considering what it represents, as seen in this table.
When it comes to the body, if Yang is the “fire”, then Yin is what serves as the water, moisture, lubricants of the body. Yin is responsible for the cooling and moistening functions of internal organs. When Yin in your body is depleted, you would feel the same as if you didn’t have a good night sleep – you don’t feel replenished and restored.
If we keep “running on empty” for a long time, or suffer a prolonged illness, our energy reserves will start to burn up and we might develop what is called “Empty Heat/Fire”. It can feel like a day when there’s a heat-wave – you’re overheating and crave a room with A/C. Developing a Yin deficiency can take years depending on one’s constitution (the energy we were born with) and environmental influences.
One of the best ways to replenish Yin is sleep, eat nourishing meals, relaxation e.g. to massage, meditation, breathing exercises like Wim Hof or Pranayama, and slow meditative movement like Yin Yoga, Qi Gong, Nei Gong or Tai Qi. The simple rule is that in order to maintain Yang, you do more high intensity physical movement/activity, and to replenish Yin, you must rest, slow down and engage in restorative actions.
When it comes to nourishment, the below are the recommended Yin tonifying foods:
Asparagus, Artichoke, Apple, Apricot, Avocado, Banana, Beans (Kidney, Lima, Black, Mung, Soy, Pea), Broccoli sprouts, Flax/Linseed, Hemp seed, Honey, Kamut, Lemon, Malt, Mango, Millet, Nettle, Pear, Pineapple, Plant milks (Soya, Coconut), Pomegranate, Pine kernel, Raspberry, Seaweed (Kelp, Nori, Wakame), Sesame seeds, Strawberry, Spelt, Spinach, Sweet Potato, Tofu, Tomato, Watermelon, Wood Ear (Black fungus), Yam.
Some of the best Yin (& blood) Tonifying herbs and spices:
Black and White Mulberry, Chinese Jujube date, Goji Berries, American ginseng, Hawthorn berry, Longan Fruit, Lily Bulb, Angelica root, Rehmania-Foxglove root, Marjoram, Arnica, Chrysanthemum, Comfrey, Hops, Red clover, Slippery Elm.
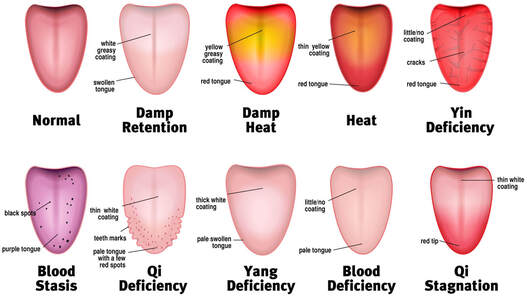
Yin Deficiency (Xu) shows on the tongue as: potential cracks, little or no coating and potentially more reddish hue
To support your body with replenishing Yin, here are some simple rules:
- Do not flood the system with excessive liquids as this might create Dampness.
- When you have a Yin deficiency, you must also avoid certain foods such as stimulants like caffeine, and foods like alcohol, refined sugar, and chilli. These foods / substances give us temporary energy (more of a Yang nature) but further deplete Yin and even worse, create potential empty heat which could develop into full internal Heat (which further exhausts Yin).
- Most Yin forming foods are also cool in nature, so be careful how you prepare the food, especially during winter. Do not eat your fruit cold directly out of the fridge or consume cold drinks - this will further tax the Spleen – which in Chinese medicine, is the organ energetically responsible for transporting and transforming nourishment around the body.
- Yin foods also tend to be raw or eaten raw, and this if taken for prolonged time – could injure the spleen or weaken it. Therefore, have a balance of raw and cooked food. Also, depending on one’s individual condition, the weaker you or your spleen is, the harder it might be to digest raw foods. So do not over-flood your system for instance with 1 litre of raw celery juice, drink 250 ml instead and gradually over time you get your nutrients absorbed while not over-burdening your spleen
- We also might need to be aware that just as any system can get overloaded, our digestive system can as well. There is only a certain amount of nutrition and nutrient that our bodies can readily absorb and utilise. Accordingly, while it might take a long time to deplete the reserves of Yin energy, it might take longer to replenish it. Therefore do not try to eat too much of Yin forming food in one go, rather gradually insert more of them in your diet over time.
- The Spleen ‘likes’ moist, warm, liquidy foods and prefers sweet, salty and sour tastes.
Watford Acupuncture Clinic